Author:
Oleg Panfilov
Reviewer:
Kai KnudsenUpdated:
27 August, 2025
This chapter covers plasmapheresis, including its principles, indications, procedure, and clinical applications in treating various disorders. Plasmapheresis is a treatment method that removes venous whole blood and returns everything except the plasma. Relatively uncommon. Several indications where it is first-line treatment. Severely ill patients, often with multiorgan failure. The method can cause complications that need to be managed. Good to know the principles of this treatment
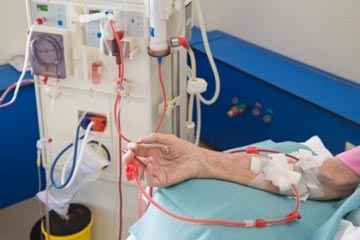
Plasmapheresis is a treatment method that removes venous whole blood and returns everything except the plasma. It does not normally remove fluid. The plasma is replaced with donor plasma or an albumin solution, usually albumin. Antibodies, immune complexes, and pathological proteins are removed. It is used in TTP/HUS, SLE, Wegener’s syndrome, Goodpasture’s syndrome, Guillain-Barré syndrome, and Myasthenia gravis. A central dialysis catheter (CDK) with a double lumen can be used acutely if vascular access is lacking, or alternatively an arterial catheter (usually in the femoral artery) and a venous catheter in the femoral vein. The treatment is performed intermittently, 3 times per week, for 2–4 hours each time. Careful weight monitoring and checking for uremia and potassium issues are important.
Plasmapheresis
- Relatively uncommon
- Several indications where it is first-line treatment
- Severely ill patients, often with multiorgan failure
- The method can cause complications that need to be managed
- Good to know the principles of this treatment
Examples of indications in the ICU:
- Guillain-Barré syndrome
- Myasthenia Gravis
- Goodpasture’s syndrome
- Catastrophic antiphospholipid syndrome (CAPS)
- Thrombotic Thrombocytopenic Purpura (TTP)
- ANCA vasculitis with pulmonary hemorrhage
- Acute liver failure
In CAPS, TTP, and ANCA vasculitis, plasmapheresis is first-line treatment.
Vid CAPS, TTP och ANCA vaskuliter är plasmaferes förstahandsbehandling

Different blood components can be separated due to differences in “specific gravity”
By centrifuging with different intensities and durations, blood can be fractionated due to differences in specific gravity.
| Component | Specific gravity |
|---|---|
| Whole blood | 1.053 |
| Erythrocytes | 1.08 |
| Platelets | 1.03 |
| Plasma | 1.02 |

Apheresis – Overview

Everything you need to know about indications…
Roughly 83 different conditions where apheresis is an appropriate treatment


Plasmapheresis
- Plasma is removed without replacement
- Example – LDL apheresis to remove cholesterol from patients who do not respond to diet and statins
- Can remove about 15% of blood volume without replacement
TPE – Therapeutic Plasma Exchange
- Plasma is removed from the patient
- Replaced with some type of replacement solution
- Always removes a pathological component
- Depending on the replacement solution, important proteins may be supplied
- Allows for administration of large volumes of donor plasma
- In immune-mediated conditions – always used together with immunosuppression
Catastrophic Antiphospholipid Syndrome (CAPS)
- Asherson’s syndrome defined in 1992
- Accelerated thrombus formation with microcirculation involvement
Definition:
- Thromboses in more than 3 organs with disturbed microcirculation
- Positive antiphospholipid antibodies
- Develops within 7 days
- Mortality up to 50% with delayed treatment
- Mortality up to 75% if untreated
Pathophysiology of CAPS
Anti-beta-2 glycoprotein affects monocytes and endothelial cells. Endothelial cells produce E-selectin and various adhesion molecules; both monocytes and endothelial cells produce tissue factor. Platelets are activated and express glycoprotein IIb and synthesize thromboxane.

TPE Treatment for CAPS
- TPE to remove antibodies, cytokines, and complement
- Every day or every other day
- 1–1.5 plasma volume
- Fresh frozen plasma as replacement
Thrombotic Thrombocytopenic Purpura – TTP
- Moschowitz syndrome discovered in 1924
- A 16-year-old girl presented with fever, low platelets, general malaise, focal neurological symptoms, and died a few days later
- The five cardinal symptoms identified in 1967 – the so-called pentad
- Mortality was over 90%
- TPE as possible treatment in 1991 – mortality reduced to just 10%
Patophysiology of TTP

Thrombocytopenic Purpura – TTP

Pathophysiology of TTP
- 80% due to antibodies against ADAMTS13
- 10% due to congenital deficiency of ADAMTS13
- Remaining are secondary TTP
- ADAMTS13 deficiency – vWF activates platelets – thrombus formation
- Exacerbated by complement system activation
TPE, TPE, TPE
- Replaces ADAMTS13 – corrects deficiency
- Washes out antibodies against ADAMTS13
- Large volumes required
- If plasmapheresis is not available – FFP transfusion can be used
TPE – Therapeutic Plasma Exchange


What is removed?
- Immunoglobulins (IgG, IgA, IgM)
- Immune complexes
- Cytokines
- M-component
- Albumin
- Coagulation factors and fibrinogen
- Electrolytes

Filtration
- Used by nephrology – plasma filter on a dialysis machine
- Requires relatively high flow – 100–200 ml/min
- Requires dialysis catheter – 12 or 13.5 Fr, 20 cm in length
- Anticoagulation – heparin or citrate
- “Plasma removal efficiency” – between 27% and 52%
- Low PRE means longer treatment times and requires higher flows – activates coagulation more

Centrifuge-based technique
- Used in hematology – special machine
- Can separate all fractions
- Low flows – 30–50 ml/min
- Peripheral access sufficient – 2 green needles
- Citrate used locally as anticoagulant
- Plasma removal efficiency – 85–87%
What replacement solutions exist?
- Crystalloids – normal saline, Ringer’s acetate
- Albumin
- Fresh frozen plasma (FFP)
Choice depends on the number of TPE sessions, frequency, and indication
Up to 30% of the volume can be replaced with crystalloids – not more, otherwise difficult hypotension due to fluid shifts; also, risk of fibrinogen and coagulation factor deficiency if TPE is frequent with short intervals
Large amounts of albumin can cause acidosis
FFP – risk of anaphylactoid reactions, expensive, transfusion risks

How are lab results affected?
- CRP decreases after TPE
- Creatinine decreases after TPE
- Bilirubin decreases after TPE
Do not take new blood samples until the next day
How many treatments and what intervals?
- Depends on pathogenesis and antibody type
- For example, in Guillain-Barré – anti-ganglioside IgG antibodies – 5–6 times every other day
- Waldenström’s macroglobulinemia – IgM antibodies – 1–3 treatments for symptom relief or before rituximab



Factors that affect treatment

How much volume should be exchanged?


Example calculation:
- 42-year-old woman, weight 52 kg
- Hematocrit 18%
- TTP patient scheduled for TPE
- EPV = (0.065 × weight) × (1 − hematocrit)
- (0.065 × 50 kg) × (1 − 0.18) = 2.7 L
- For TTP, FFP is given as replacement – thus in ICU we need to order 2.7 L FFP before treatment
Complications
How is drug delivery affected?

Drug properties
TPE prescription depends on:
- Volume of distribution – Vd < 0.2 L/kg
- High Vd – less affected
- Protein binding
- High protein binding – more affected
- In ICU, Vd changes due to fluid shifts, etc.
- High protein binding – highly affected, low protein binding – less affected
- If a drug is given just before TPE – high plasma concentration – more affected
TPE prescription
- Timing of administration
- Duration
- Interval between TPE sessions
- Volume exchanged
- Replacement fluid
Specific drug examples
| Drug | Protein Binding | Vd (L/kg) | Adjusted Dose |
|---|---|---|---|
| Cortisone | 90–95% | 0.6–0.7 | No |
| Cyclosporin | 98% | 13 | No |
| Tacrolimus | Very high | Large | No |
| Aspirin | 90% | 0.1 | Yes |
| LMW Heparin | – | – | Yes |
| Acyclovir | 15% | 0.69 | No |
| Tobramycin | 10% | 0.25 | Affected by Ca2+ concentration |
| Vancomycin | 70% | 0.39 | Measure concentration |
Immunosuppression and TPE
Drug recommendations
- In principle – most drugs should be administered after TPE
- Measure concentrations where possible
- Wait 24–36 hours before next TPE session




Examples of indications for immunoadsorption:
- Before or after ABO-incompatible liver transplant
- Pemphigus
- Familial hypercholesterolemia (homozygous)
- SLE
- Many new indications in the future

High-volume TPE in acute liver failure
- Removes protein-bound toxins, ammonia, endotoxins, mercaptans, phenols, etc.
- Lower risk of cerebral edema
- Less SIRS and vasoplegia
- Improved coagulation
High-volume TPE in acute liver failure
- Every day (in studies: 3 days)
- 8–12 L plasma exchanged
- To bridge to liver transplant or improvement
- Lab samples taken at least 12 hours after TPE
High-flow plasmapheresis (TPE) and liver injury

Disclaimer:
The content on AnesthGuide.com is intended for use by medical professionals and is based on practices and guidelines within the Swedish healthcare context.
While all articles are reviewed by experienced professionals, the information provided may not be error-free or universally applicable.
Users are advised to always apply their professional judgment and consult relevant local guidelines.
By using this site, you agree to our Terms of Use.